Cytogenetics
Cytogenetics is a branch of genetics that is concerned with the study of the structure and function of the cell…cytogenetics of male and female reproductive physiology means study of the structure and functions of the cells related to reproductive activity — in male : sertoli cells,leydig cells and sperm(germ cell);in female : follicular cell (primordial follicle to ova — female reproductive cycle)
The female reproductive system is designed to carry out several functions. It produces the female egg cells necessary for reproduction, called the ova or oocytes. The system is designed to transport the ova to the site of fertilization. Conception, the fertilization of an egg by a sperm, normally occurs in the fallopian tubes. The next step for the fertilized egg is to implant into the walls of the uterus, beginning the initial stages of pregnancy. If fertilization and/or implantation does not take place, the system is designed to menstruate (the monthly shedding of the uterine lining). In addition, the female reproductive system produces female sex hormones that maintain the reproductive cycle.
What Parts Make up the Female Anatomy?
The female reproductive anatomy includes parts inside and outside the body.
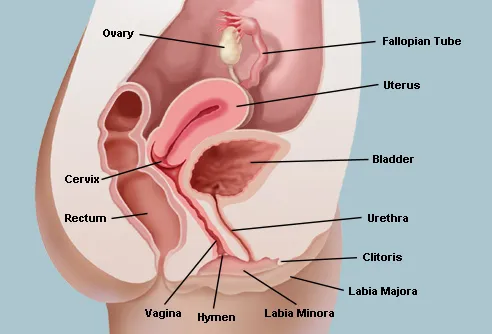
The function of the external female reproductive structures (the genitals) is twofold: To enable sperm to enter the body and to protect the internal genital organs from infectious organisms. The main external structures of the female reproductive system include:
- Labia majora: The labia majora enclose and protect the other external reproductive organs. Literally translated as “large lips,” the labia majora are relatively large and fleshy, and are comparable to the scrotum in males. The labia majora contain sweat and oil-secreting glands. After puberty, the labia majora are covered with hair.
- Labia minora: Literally translated as “small lips,” the labia minora can be very small or up to 2 inches wide. They lie just inside the labia majora, and surround the openings to the vagina (the canal that joins the lower part of the uterus to the outside of the body) and urethra (the tube that carries urine from the bladder to the outside of the body).
- Bartholin’s glands: These glands are located beside the vaginal opening and produce a fluid (mucus) secretion.
- Clitoris: The two labia minora meet at the clitoris, a small, sensitive protrusion that is comparable to the penis in males. The clitoris is covered by a fold of skin, called the prepuce, which is similar to the foreskin at the end of the penis. Like the penis, the clitoris is very sensitive to stimulation and can become erect.
The internal reproductive organs in the female include:

- Vagina: The vagina is a canal that joins the cervix (the lower part of uterus) to the outside of the body. It also is known as the birth canal.
- Uterus (womb): The uterus is a hollow, pear-shaped organ that is the home to a developing fetus. The uterus is divided into two parts: the cervix, which is the lower part that opens into the vagina, and the main body of the uterus, called the corpus. The corpus can easily expand to hold a developing baby. A channel through the cervix allows sperm to enter and menstrual blood to exit.
- Ovaries: The ovaries are small, oval-shaped glands that are located on either side of the uterus. The ovaries produce eggs and hormones.
- Fallopian tubes: These are narrow tubes that are attached to the upper part of the uterus and serve as tunnels for the ova (egg cells) to travel from the ovaries to the uterus. Conception, the fertilization of an egg by a sperm, normally occurs in the fallopian tubes. The fertilized egg then moves to the uterus, where it implants into the lining of the uterine wall.
What Happens During the Menstrual Cycle?
Females of reproductive age experience cycles of hormonal activity that repeat at about one-month intervals. With every cycle, a woman’s body prepares for a potential pregnancy, whether or not that is the woman’s intention. The term menstruation refers to the periodic shedding of the uterine lining. (Menstru means “monthly.”)
The average menstrual cycle takes about 28 days and occurs in phases: the follicular phase, the ovulatory phase (ovulation), and the luteal phase.
There are four major hormones (chemicals that stimulate or regulate the activity of cells or organs) involved in the menstrual cycle: follicle-stimulating hormone(FSH), luteinizing hormone(L.H), estrogen, and progesterone.
Follicular Phase of the Menstrual Cycle
This phase starts on the first day of your period. During the follicular phase of the menstrual cycle, the following events occur:
- Two hormones, follicle stimulating hormone (FSH) and luteinizing hormone (LH), are released from the brain(Pituitary gland) and travel in the blood to the ovaries.
- The hormones stimulate the growth of about 15 to 20 eggs in the ovaries, each in its own “shell,” called a follicle.
- These hormones (FSH and LH) also trigger an increase in the production of the female hormone estrogen.
- As estrogen levels rise, like a switch, it turns off the production of follicle-stimulating hormone. This careful balance of hormones allows the body to limit the number of follicles that mature.
- As the follicular phase progresses, one follicle in one ovary becomes dominant and continues to mature. This dominant follicle suppresses all of the other follicles in the group. As a result, they stop growing and die. The dominant follicle continues to produce estrogen.

Ovulatory Phase of the Menstrual Cycle
The ovulatory phase, or ovulation, starts about 14 days after the follicular phase started. The ovulatory phase is the midpoint of the menstrual cycle, with the next menstrual period starting about two weeks later. During this phase, the following events occur:
- The rise in estrogen from the dominant follicle triggers a surge in the amount of luteinizing hormone that is produced by the brain.
- This causes the dominant follicle to release its egg from the ovary.
- As the egg is released (a process called ovulation), it is captured by finger-like projections on the end of the fallopian tubes (fimbriae). The fimbriae sweep the egg into the tube.
- Also during this phase, there is an increase in the amount and thickness of mucus produced by the cervix (lower part of the uterus). If a woman were to have intercourse during this time, the thick mucus captures the man’s sperm, nourishes it, and helps it to move towards the egg for fertilization.
Luteal Phase of the Menstrual Cycle
The luteal phase of the menstrual cycle begins right after ovulation and involves the following processes:
- Once it releases its egg, the empty follicle develops into a new structure called the corpus luteum.
- The corpus luteum secretes the hormone progesterone. Progesterone prepares the uterus for a fertilized egg to implant.
- If intercourse has taken place and a man’s sperm has fertilized the egg (a process called conception), the fertilized egg (embryo) will travel through the fallopian tube to implant in the uterus. The woman is now considered pregnant.
- If the egg is not fertilized, it passes through the uterus. Not needed to support a pregnancy, the lining of the uterus breaks down and sheds, and the next menstrual period begins.
How Many Eggs Does a Woman Have?
The vast majority of the eggs within the ovaries steadily die, until they are depleted at menopause. At birth, there are approximately 1 million to 2 million eggs; by the time of puberty, only about 300,000 remain. Of these, only about 500 will be ovulated during a woman’s reproductive lifetime. Any remaining eggs gradually die out at menopause.
Serogenetics
Serogenetics is branch of genetics that is concerned with study of serological proteins.Serogenetics of male and female reproductive physiology means the study of serum harmones which regulate the formation of germ cells.(gonadotropins-FSH,LH,HCG and sex harmones – Testosterone, estrogen and progesterone)
There are five main hormones that control the menstrual cycle. Three are produced in the brain, while the other two are made in the ovaries.
- Gonadotrophin-releasing hormone (GnRH) is made by a part of the brain called the hypothalamus. GnRH travels to another part of the brain where it controls the release of follicle-stimulating hormone (FSH) and luteinising hormone (LH).
- FSH is released by a part of the brain called the anterior pituitary. FSH is carried by the bloodstream to the ovaries. Here it stimulates the immature eggs (ova) to start growing.
- LH is also released by the anterior pituitary and travels to the ovaries. LH triggers ovulation and encourages the formation of a special group of cells called the corpus luteum.
- Oestrogen is produced by the growing ova and by the corpus luteum. In moderate amounts oestrogen helps to control the levels of GnRH, FSH and LH. This helps to prevent the development of too many ova. Oestrogen also helps to develop and maintain many of the female reproductive structures.
- Progesterone is mainly released by the corpus luteum. It works with oestrogen to thicken the lining of the uterus ready for the implantation of a fertilised ovum. It also helps to prepare the breasts for releasing milk. High levels of progesterone control the levels of GnRH, FSH and LH.
During the last few days of the menstrual cycle, around 20 small immature ova begin to develop in the ovaries. This continues throughout the menstrual cycle. FSH and LH encourage the growth of these ova. As they grow, the ova also start to release increasing amounts of oestrogen. The amount of oestrogen produced reduces the amount of FSH released. This helps to prevent too many ova growing at the same time. Eventually one ovum outgrows the rest.
While this is happening in the ovaries, the oestrogen produced also causes a thickening of the lining of the uterus.
What is ovulation?
Ovulation is the stage in the menstrual cycle when the mature ovum is released from the ovaries into the Fallopian tubes. By this point in the cycle, levels of oestrogen are high. Previously, medium levels of oestrogen reduced the amount of FSH and LH released. Now this high level of oestrogen is the signal for more FSH and LH to be released. LH causes the ovum to burst through the outer layer of the ovary. Usually the ovum is then swept into the uterine tubes.
When the ovum leaves the ovary, the cells left behind become the corpus luteum. This special group of cells is capable of producing several different hormones, including progesterone and oestrogen. These hormones encourage the growth and maturation of the lining of the uterus.
What happens next depends on whether the ovum is fertilised by sperm. If the ovum is fertilised, the corpus luteum continues to produce hormones. Another hormone called human chorionic gonadotrophin (hCG) stops the corpus luteum from breaking down. The cells covering the embryo produce hCG. It is the hormone detected in pregnancy tests.
If the ovum is not fertilised, the corpus luteum can only live for a further two weeks. As it begins to break down, it releases fewer of its hormones. As the levels of progesterone and oestrogen go down, they no longer control the levels of GnRH, FSH and LH. So, these hormones increase and new ova begin to develop – the start of a new menstrual cycle. In the uterus the decrease in progesterone stimulates the release of chemicals that eventually cause the lining of the uterus to die off. This is the blood flow experienced during menstruation.